
How to Stop Period Cramps Fast: 12 Remedies That Actually Work
From ibuprofen to heat pads — 12 evidence-backed ways to beat period cramps quickly.
If your stomach takes a nosedive every time your period starts, you're not imagining it — and you're far from alone. Here's the science, and what actually helps.

Rushing to the bathroom the moment your period arrives is so common it has a nickname among gynaecologists: "period poos." Research suggests roughly 73% of women experience gastrointestinal symptoms — including diarrhea, nausea, or bloating — during menstruation. It is not a coincidence, a food sensitivity, or anxiety. It is biology, and the culprit has a name: prostaglandins.
How prostaglandins cause period diarrhea
Prostaglandins are hormone-like lipid compounds made in many tissues throughout the body. During menstruation, the uterine lining produces large amounts of two types — PGE2 and PGF2α — to trigger the muscle contractions that push the lining out.
The problem is that prostaglandins don't stay local. They enter the bloodstream and act on smooth muscle anywhere they travel. The intestines are lined with smooth muscle, and when prostaglandins bind to receptors there, they accelerate intestinal transit — meaning your body moves stool through much faster than usual, resulting in loose stools or full diarrhea.
Women with heavier periods and stronger cramps tend to produce more prostaglandins — and also tend to experience more severe GI symptoms. This is why ibuprofen (an NSAID that blocks prostaglandin production at the source) helps both cramps and period diarrhea.
When endometrial-like tissue grows on or near the bowel or rectum, it responds to hormonal changes just like the uterine lining — bleeding, swelling, and inflaming during menstruation. This causes severe diarrhea, bowel pain, and sometimes visible rectal bleeding during your period. Endometriosis affects approximately 1 in 10 women of reproductive age and is significantly underdiagnosed — average diagnosis time is 7–10 years.
Medical conditionIBS affects approximately 15% of the population and is significantly more common in women. Research shows that up to 50% of women with IBS report their symptoms worsen during menstruation — a direct result of prostaglandins amplifying an already-sensitive gut. If you have loose stools, urgency, or cramping outside of your period too, IBS may be a co-existing factor worth discussing with a doctor.
Medical conditionProgesterone — which peaks in the second half of your cycle and then drops sharply before your period — has a relaxing effect on smooth muscle, including the gut wall. When progesterone falls, this relaxing effect disappears and the gut becomes more reactive. Foods that you can normally tolerate (caffeine, dairy, spicy foods) may trigger loose stools during your period because your gut sensitivity is already elevated.
Lifestyle factorThe gut and brain are connected via the vagus nerve and the enteric nervous system. Pre-menstrual anxiety or mood changes can directly stimulate gut motility through this axis. Research shows that perceived stress in the days before menstruation correlates with more severe GI symptoms during the period itself — independent of prostaglandin levels. Managing stress in your luteal phase can genuinely reduce period diarrhea.
Lifestyle factorMagnesium levels naturally drop in the days before menstruation. Low magnesium is associated with both increased muscle excitability (contributing to cramps) and altered gut motility. Some research suggests that magnesium supplementation (200–400 mg daily) taken throughout the luteal phase can reduce both the frequency and severity of period-related GI symptoms, as well as premenstrual cramping.
Often overlooked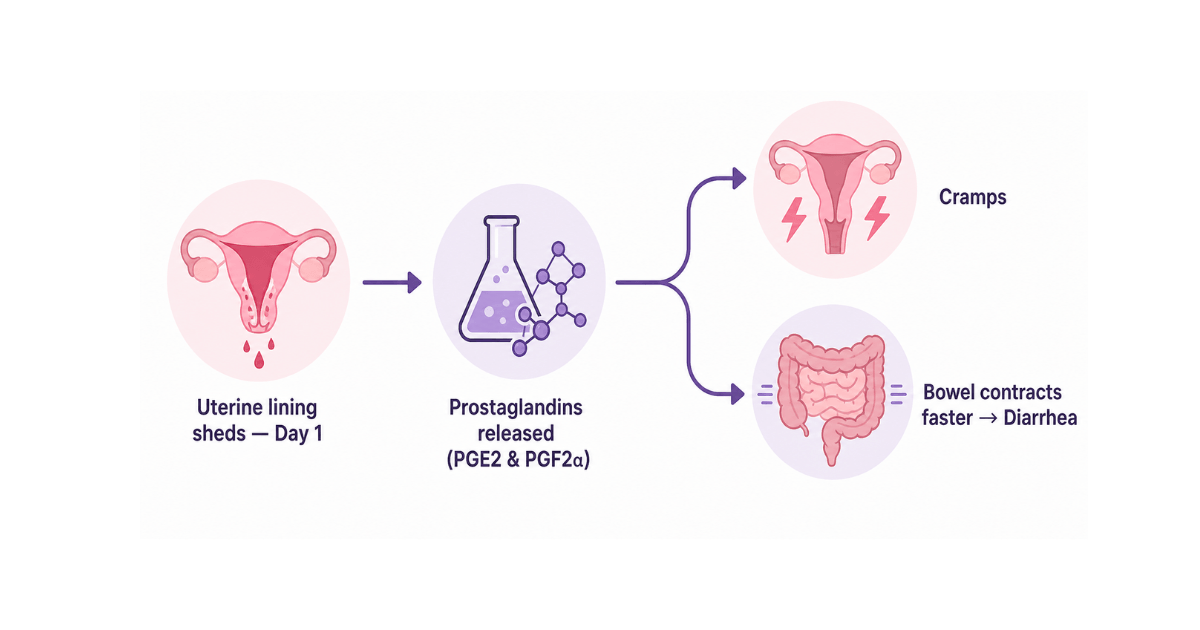
Most period diarrhea resolves on its own within 1–2 days. But you don't have to just wait it out. These strategies range from immediate relief to longer-term prevention:

Most period diarrhea is a straightforward prostaglandin response. But certain patterns signal that something else is going on:
Track your symptoms with Wamiga
Log GI symptoms, flow, and pain every day. Wamiga spots patterns across cycles so you can show your doctor exactly what's happening.