Getting Your Period Twice a Month — What Does It Mean?
Short cycle, ovulation spotting, or fibroids? Here are the 9 most common causes of bleeding twice a month.
A period that vanishes in a day or two can feel alarming — or like a blessing. Either way, your cycle is handing you a signal worth understanding.
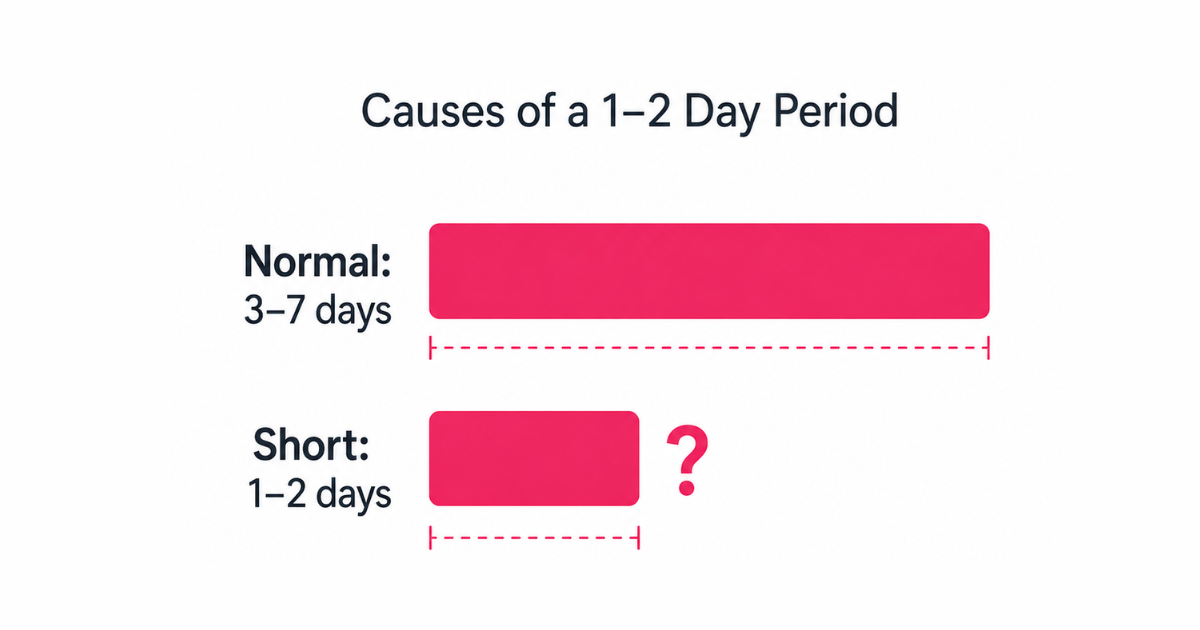
A "normal" period lasts between 2 and 7 days, according to the American College of Obstetricians and Gynecologists (ACOG). If yours wraps up in a day or two — or feels lighter than a tissue — it can be perfectly fine, or it can point to something that deserves attention.
The medical term for an unusually short or light period is hypomenorrhea. It covers any menstruation that is noticeably briefer or lighter than what's typical for you. Below you'll find the eight most common reasons — from the completely harmless to the ones worth investigating.
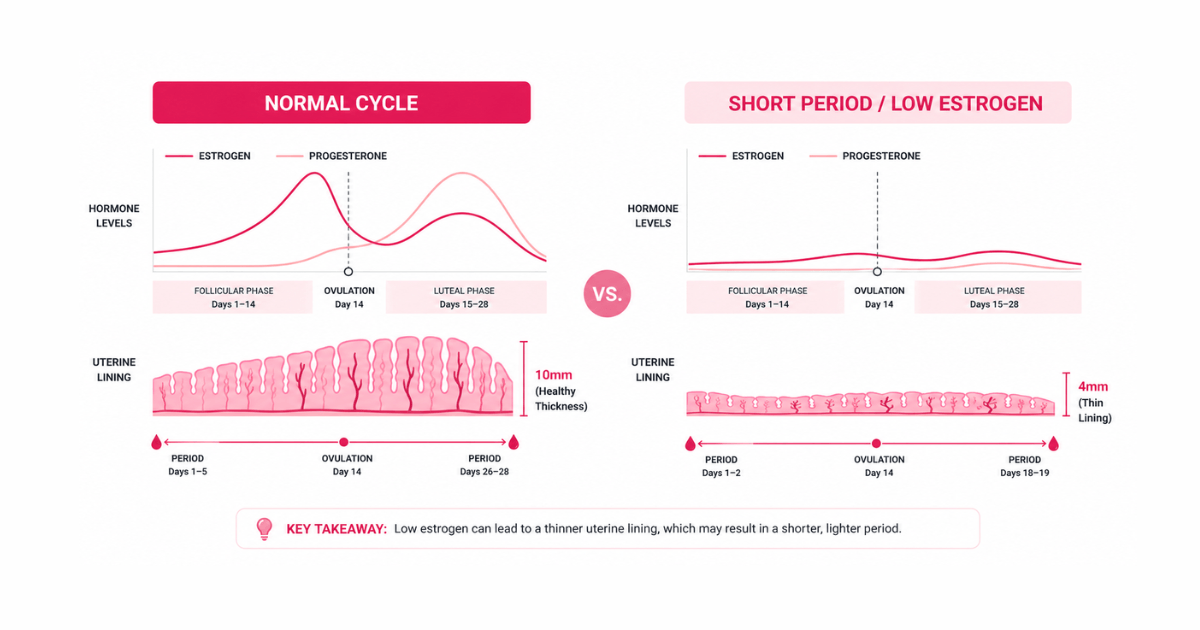
Your uterine lining (endometrium) builds up throughout the first half of your cycle under the influence of estrogen. If estrogen levels are low, the lining stays thin — sometimes only 4–6 mm rather than the typical 7–16 mm. Less lining means less to shed, which means a shorter, lighter bleed. Low estrogen can stem from overexercise, undereating, perimenopause, or primary ovarian insufficiency.
HormonalThe mini-pill (progestin-only), hormonal IUS (Mirena, Kyleena), the contraceptive implant, and even the combined pill can all significantly reduce the amount and duration of bleeding. The hormonal IUS, for example, thins the uterine lining so much that roughly 20% of users stop having periods altogether after one year. A 1–2 day bleed on any hormonal method is completely expected and is not a sign of pregnancy on its own.
Very commonWhen you're under sustained stress, your adrenal glands release cortisol. High cortisol suppresses the hypothalamic signal (GnRH) that drives your entire reproductive cycle. Lower GnRH means lower FSH and LH, which means a weaker ovulation signal and a thinner lining — and a shorter period as a result. Exam weeks, relationship difficulties, work deadlines, and bereavement are all recognised triggers.
LifestyleFat tissue converts androgens into estrogen. When body fat drops below a critical threshold — commonly seen in distance runners, gymnasts, and people with restrictive eating disorders — circulating estrogen falls sharply. This is called hypothalamic amenorrhea in its most severe form, but milder versions cause noticeably short, light periods long before periods stop entirely. Relative Energy Deficiency in Sport (RED-S) is the modern clinical framework for this pattern.
Lifestyle
PCOS is most often associated with heavy, irregular periods — but not always. Some women with PCOS have elevated androgens that suppress estrogen's lining-building effect, leading to a thin endometrium and consequently short, light periods. Others have anovulatory cycles where no egg is released: without ovulation, progesterone never rises and the lining never fully matures, resulting in irregular spotting rather than a true period. PCOS affects approximately 1 in 10 women of reproductive age.
Medical conditionYour thyroid gland influences virtually every hormonal process in the body. Hypothyroidism (underactive thyroid) is more often linked to heavy periods, but hyperthyroidism (overactive thyroid) commonly causes scanty, short periods. Thyroid disorders also disrupt prolactin and sex-hormone-binding globulin (SHBG) levels, indirectly altering how much estrogen is biologically available. Thyroid issues affect approximately 1 in 8 women during their lifetime and are easily screened with a simple blood test (TSH).
Medical conditionPerimenopause — the transition into menopause — typically begins in a woman's mid-to-late 40s, though it can start earlier. As ovarian estrogen production becomes erratic, cycles become unpredictable: sometimes heavier and longer, sometimes scanty and brief. A period that has noticeably shortened after age 40 without an obvious lifestyle explanation is worth discussing with a doctor, especially if you're also experiencing hot flashes, sleep disruption, or mood changes.
HormonalImplantation bleeding occurs when a fertilised egg embeds in the uterine lining, typically 10–14 days after conception — which can coincide with when your period would be due. Unlike a true period, it's usually pink or light brown, lasts 1–3 days, and is noticeably lighter than a typical bleed. If your "period" arrived on time but was unusually short and light, take a pregnancy test. Home tests are reliable from the first day of a missed period.
Check firstContext matters enormously. A 2-day period that you've always had is very different from a period that used to last 5 days and has recently dropped to 1. Use the guide below to orient yourself:
If your periods became suddenly and dramatically shorter or stopped after a uterine procedure — such as a dilation and curettage (D&C), fibroid removal, or caesarean section — Asherman's syndrome is worth ruling out. This is a condition where scar tissue (intrauterine adhesions) forms inside the uterine cavity, reducing the functional surface area that bleeds each month. It's uncommon, but it is a correctable cause of hypomenorrhea. A gynaecologist can diagnose it with a hysteroscopy or sonohysterogram.
Short periods are usually not an emergency, but the following situations deserve a medical conversation:
Your doctor will likely start with a blood panel checking FSH, LH, estradiol, prolactin, TSH, and possibly androgens — this covers most hormonal causes in a single visit.
Depending on the cause, several approaches can help restore a fuller period:
Track your cycle with Wamiga
Log your flow, duration, and symptoms every day. Spot patterns that help you and your doctor understand what's normal for you.