
How to Stop Period Cramps Fast: 12 Remedies That Actually Work
From ibuprofen to heat pads — 12 evidence-backed ways to beat period cramps quickly.
That aching lower back every time your period starts isn't just bad luck — it's your uterus and your nervous system doing something completely predictable. Here's the science and 7 evidence-based ways to stop it.
You wake up on day one of your period and your lower back is already aching before you've even gotten out of bed. It feels like someone tightened a belt around your pelvis and lower spine overnight. If this happens to you every single cycle, you're not imagining it — and you're far from alone.
Studies estimate that up to 72% of women who experience period pain also have back pain as part of the picture. For most women, this pain is completely explainable and manageable. For some, it's a signal worth investigating. The key is knowing which type you're dealing with — and this guide will help you figure that out.
Whether your back pain is a dull ache that tracks with your cramps, a sharp stabbing sensation, or a radiating pain that shoots down your legs, the information below covers the mechanism, the causes, and seven evidence-backed methods to actually feel better.
The most important thing to understand about period back pain is that it is, in most cases, referred pain — meaning the pain originates in your uterus but your brain registers it as coming from your lower back. This isn't unusual. The same mechanism is why a heart attack can cause left arm pain, even though nothing is wrong with the arm.
Your uterus and your lower back share overlapping nerve supply pathways. Specifically, the T10 to L1 dermatomes — segments of the spinal cord — receive pain signals from both the uterus and the lower back skin and muscles. When your uterus contracts intensely during menstruation, the pain signal travels up these shared nerve routes, and your brain can't always tell exactly where it came from. The result: you feel it in your back.
In addition to referred pain, the physical act of uterine contractions can also cause direct muscle tension in the surrounding pelvic floor muscles, hip flexors, and lower back muscles — adding a real muscular component on top of the referred nerve pain.
The trigger for most period pain — including the back pain — is a class of hormone-like compounds called prostaglandins, specifically PGF2α and PGE2. They are released by the endometrium (uterine lining) as it begins to shed at the start of your period.
Prostaglandins serve a useful purpose: they tell your uterine muscles to contract, which pushes the lining out. The problem is that higher concentrations of prostaglandins cause more powerful, more frequent contractions — and more intense pain. Women with primary dysmenorrhea have been shown in studies to have measurably higher prostaglandin concentrations in their endometrial tissue compared to women without pain.
Not all period back pain has the same cause. Doctors classify painful periods into two categories, and knowing which one applies to you changes what you should do about it.
Where your back pain is, what it feels like, and how it behaves over your cycle can all give important clues about what's causing it. Here are the three most common patterns:
A persistent, low-level ache across the lower back that comes and goes with cramps. Peaks on days 1–2 and fades as the period progresses.
Usually: Primary DysmenorrheaSudden, intense bursts of pain in the lower back or sacral area, often in sync with uterine cramps. Can be severe on day 1.
Usually: High ProstaglandinsPain that moves from the lower back down through the hips, buttocks, or legs. Often associated with endometriosis pressing on sacral nerves.
May Signal: EndometriosisUnderstanding the root cause of your back pain helps you choose the right treatment — and know when to see a doctor.
The most common cause. High prostaglandin levels at the start of your period trigger strong uterine contractions. These contractions cause referred pain along the T10–L1 nerve pathways, registering as lower back pain. Pain typically peaks on day 1–2 and resolves within 2–3 days as prostaglandin levels fall.
Most CommonEndometrial-like tissue growing outside the uterus can attach to pelvic nerves, the sacrum, and the posterior pelvic wall. This creates deep, chronic back pain that often starts before the period, lasts beyond it, and progressively worsens over time. It affects approximately 10–15% of women of reproductive age and is one of the most common reasons for secondary dysmenorrhea. Back pain from endometriosis often radiates into the hips and legs.
See a DoctorAdenomyosis occurs when the endometrium grows into the muscular wall of the uterus, causing it to enlarge — sometimes up to three times its normal size. The enlarged, heavy uterus can directly compress surrounding nerves and structures, causing deep, diffuse lower back pain and pelvic pressure. It often coexists with heavy periods and is estimated to affect 20–35% of people with a uterus.
See a DoctorFibroids are benign muscle tumors that grow in or on the uterine wall. Larger fibroids can press against the lumbar spine, sacral nerves, and nearby pelvic structures, causing back pain that worsens during menstruation when blood flow to the area increases. Fibroids are very common — present in up to 70–80% of women by age 50 — though most are asymptomatic.
May Need EvaluationEven in primary dysmenorrhea, the body's response to pelvic pain often involves unconsciously tensing the lower back, hip flexors, and pelvic floor muscles to protect the painful area. This muscle tension adds a real, structural back pain component on top of the referred pain. Poor posture and spending long hours sitting during your period can amplify this significantly.
Lifestyle Factor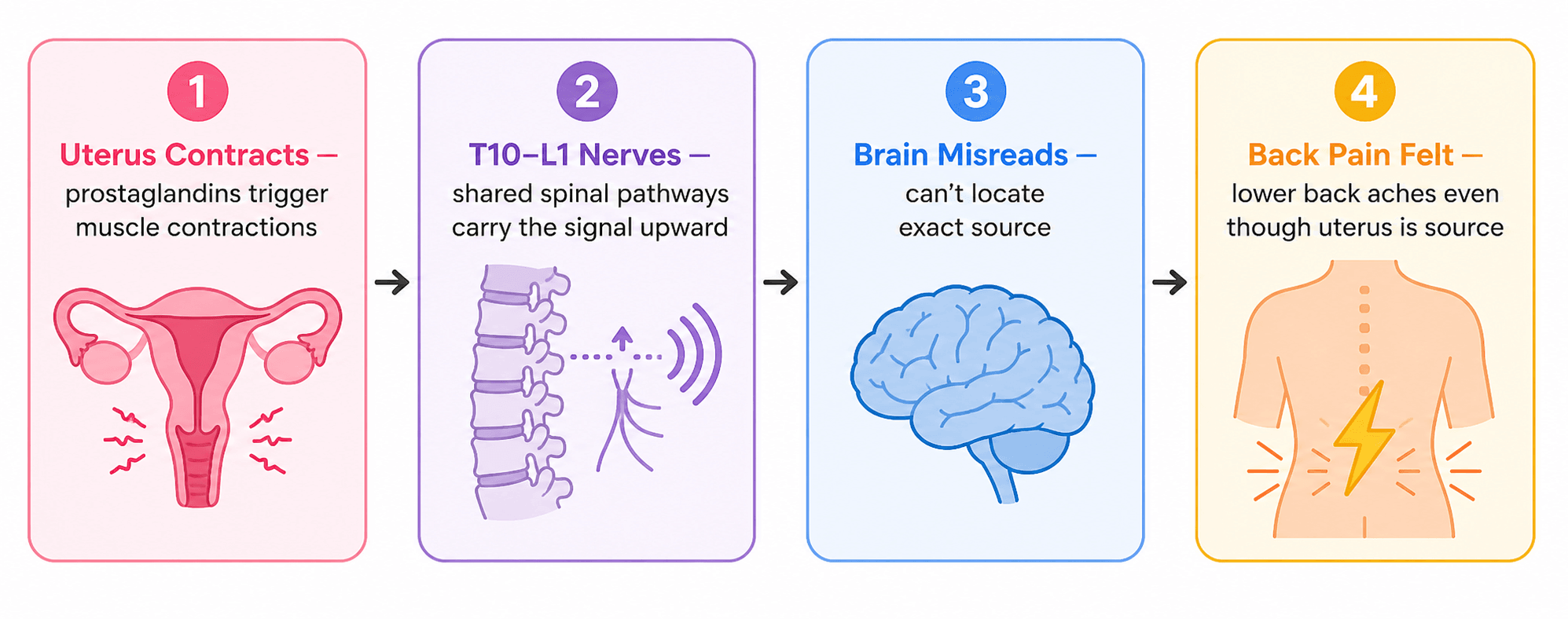
Track your cycle with Wamiga
Log daily symptoms including back pain, cramps, and mood. Spot patterns across cycles and show a doctor exactly when your pain starts — shortening the path to the right diagnosis.
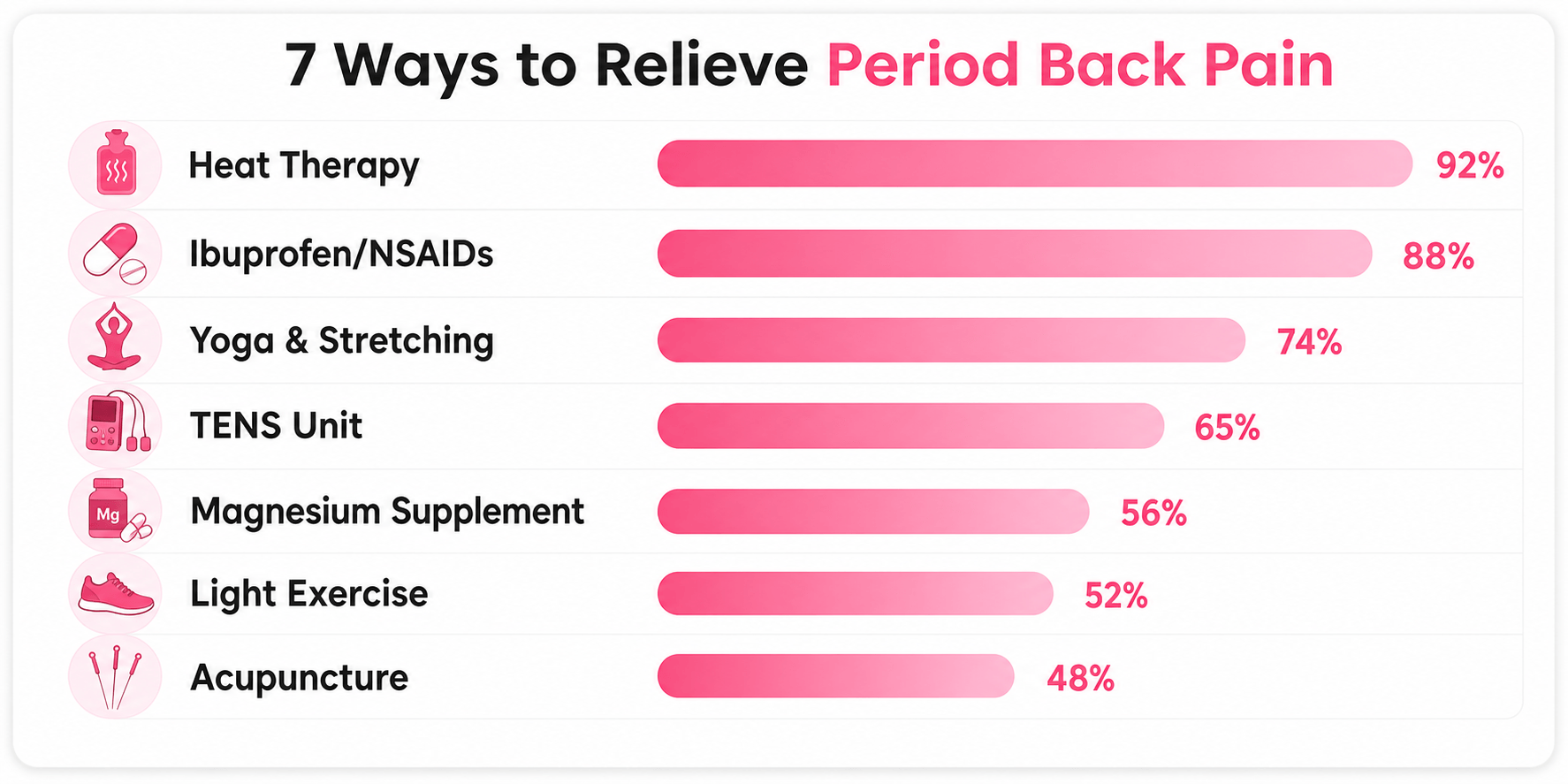
The good news: most period back pain responds well to treatment. The seven methods below are ranked loosely by evidence strength and how quickly they work.
These three poses directly target the hip flexors, pelvic floor, and lower back muscles that tighten during menstruation:
Most period back pain is primary dysmenorrhea and entirely manageable at home. But there are specific patterns that warrant a conversation with a gynaecologist — because they can indicate endometriosis, adenomyosis, or fibroids that respond to dedicated treatment.
If any of these apply to you, a gynaecologist can evaluate you with a pelvic exam and ultrasound. Endometriosis and adenomyosis are both very treatable once diagnosed — the average diagnosis delay for endometriosis is unfortunately 7–10 years, largely because women are told their pain is "just normal." It shouldn't be that disabling.
Period back pain is real, common, and — for most women — a predictable result of the prostaglandin-driven referred pain mechanism that activates every cycle. Heat therapy and ibuprofen are your fastest, most evidence-backed tools. For persistent, worsening, or radiating back pain, don't dismiss it as "just your period" — get it evaluated, because conditions like endometriosis are very treatable when caught early.
Tracking your symptoms cycle to cycle is one of the most useful things you can do. When you can show a doctor a month-by-month log of when your back pain starts, how long it lasts, and how intense it is, it dramatically shortens the path to the right diagnosis. Wamiga makes that log automatic.