In this article
What Is Ovulation Bleeding?
Ovulation bleeding — also called mid-cycle spotting or ovulation spotting — is light vaginal bleeding that occurs around the time an egg is released from the ovary. It is not a period. It is not implantation bleeding. It is a brief bleed directly caused by the hormonal and physical events of ovulation itself.
It typically appears as a pale pink or brownish tinge in your cervical mucus or on toilet paper — not flowing blood, and rarely enough to need a pad or liner. For most people who experience it, ovulation spotting is a benign, predictable event that repeats at the same mid-cycle point every month.
The key takeaway: ovulation bleeding is completely normal and requires no treatment unless it is accompanied by unusual pain, odour, or other symptoms.
How Common Is Ovulation Bleeding?
Mid-cycle spotting is real but uncommon. Research published in Fertility and Sterility found that confirmed ovulation spotting occurs in approximately 4.8% of cycles in women who track their cycles closely. One-off or occasional spotting is reported by up to 10–12% of menstruating people at some point in their reproductive years.
If you experience it consistently at the same cycle day each month, your body is likely more sensitive to the hormone shift at ovulation — completely normal. If it is new or irregular, that warrants a mention to your doctor.
Tip: Because ovulation spotting is uncommon, many women who experience it mistakenly believe something is wrong. Consistent mid-cycle spotting with no other symptoms is almost always benign — but logging it in a period tracker gives you the pattern evidence to confirm this.
What Does Ovulation Bleeding Look Like?
The appearance of ovulation spotting is the first clue that distinguishes it from a period or other bleeding. Three things make it different: colour, volume, and what it is mixed with.
The volume comparison is equally important:
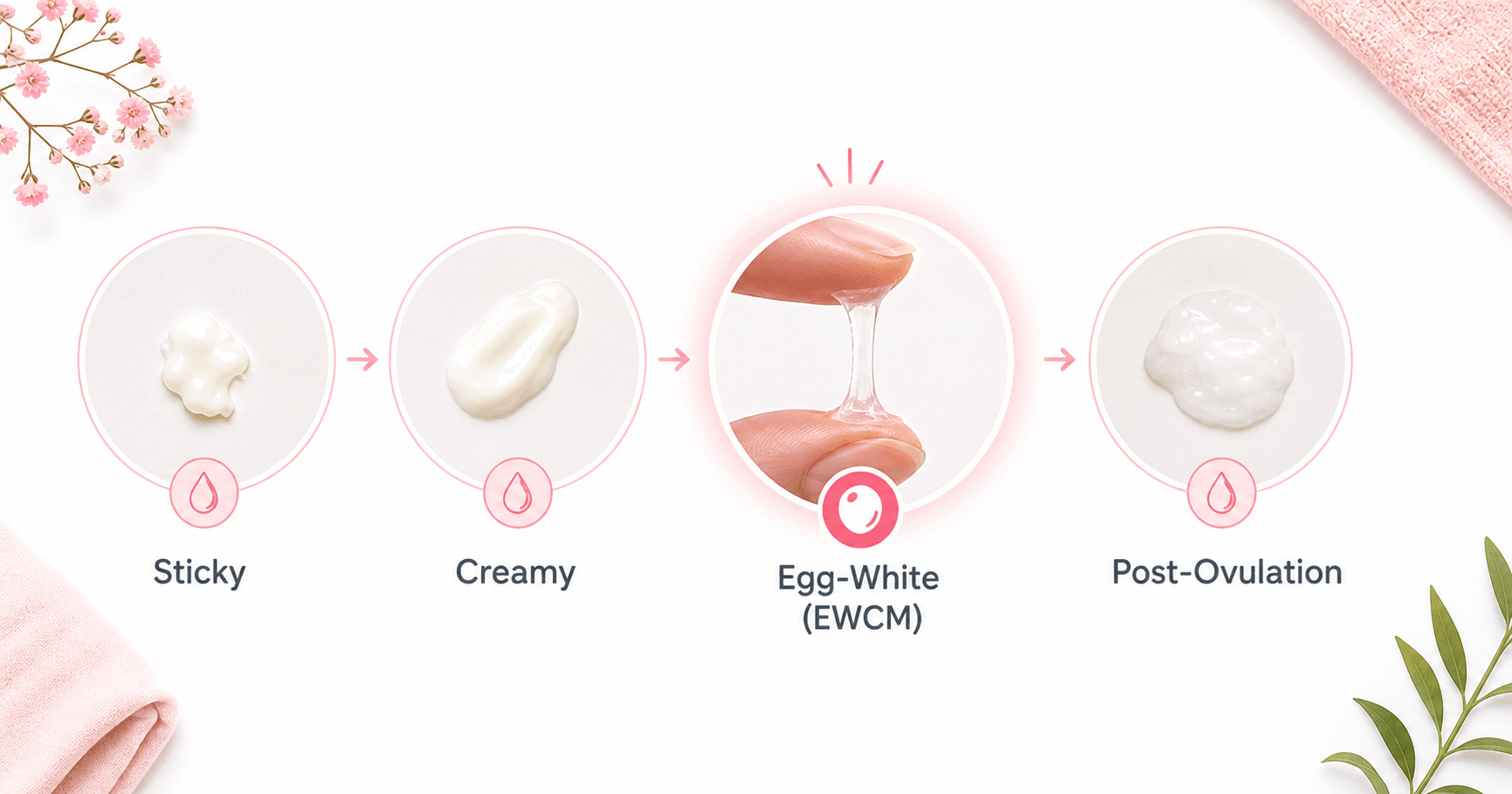
You will almost always find ovulation spotting mixed with the egg-white cervical mucus (EWCM) that is most abundant at peak fertility — giving it a pink-tinged, clear, stretchy quality. This is one of the most reliable identifiers.
Why Does It Happen? The Biology
There are three biological mechanisms behind ovulation bleeding, often occurring together:
The Follicle Ruptures
When a dominant follicle — a small fluid-filled sac in the ovary — bursts to release the egg, it creates a tiny wound on the ovary's surface. A small amount of blood and follicular fluid escapes into the pelvic cavity, travels through the fallopian tube into the uterus, and can exit through the cervix as very light spotting. This is the most direct mechanical cause.
The Estrogen Dip
In the days before ovulation, estrogen surges sharply — triggering the LH surge that causes egg release. Immediately after the LH peak, estrogen briefly falls before progesterone takes over and stabilises the uterine lining. This short estrogen withdrawal is similar (on a smaller scale) to what causes your period: the uterine lining sheds a tiny amount of blood, creating a mini-bleed that resolves within hours to a day once progesterone rises.
Heightened Cervical Sensitivity
Around ovulation, the cervix becomes softer, more open, and more vascular — all changes that support sperm entry. For some people, this increased blood flow means even minor mechanical stimulation or the surge in mucus production can cause light spotting. People with cervical ectropion (a harmless condition where inner cervical cells extend outward) are especially prone to this.
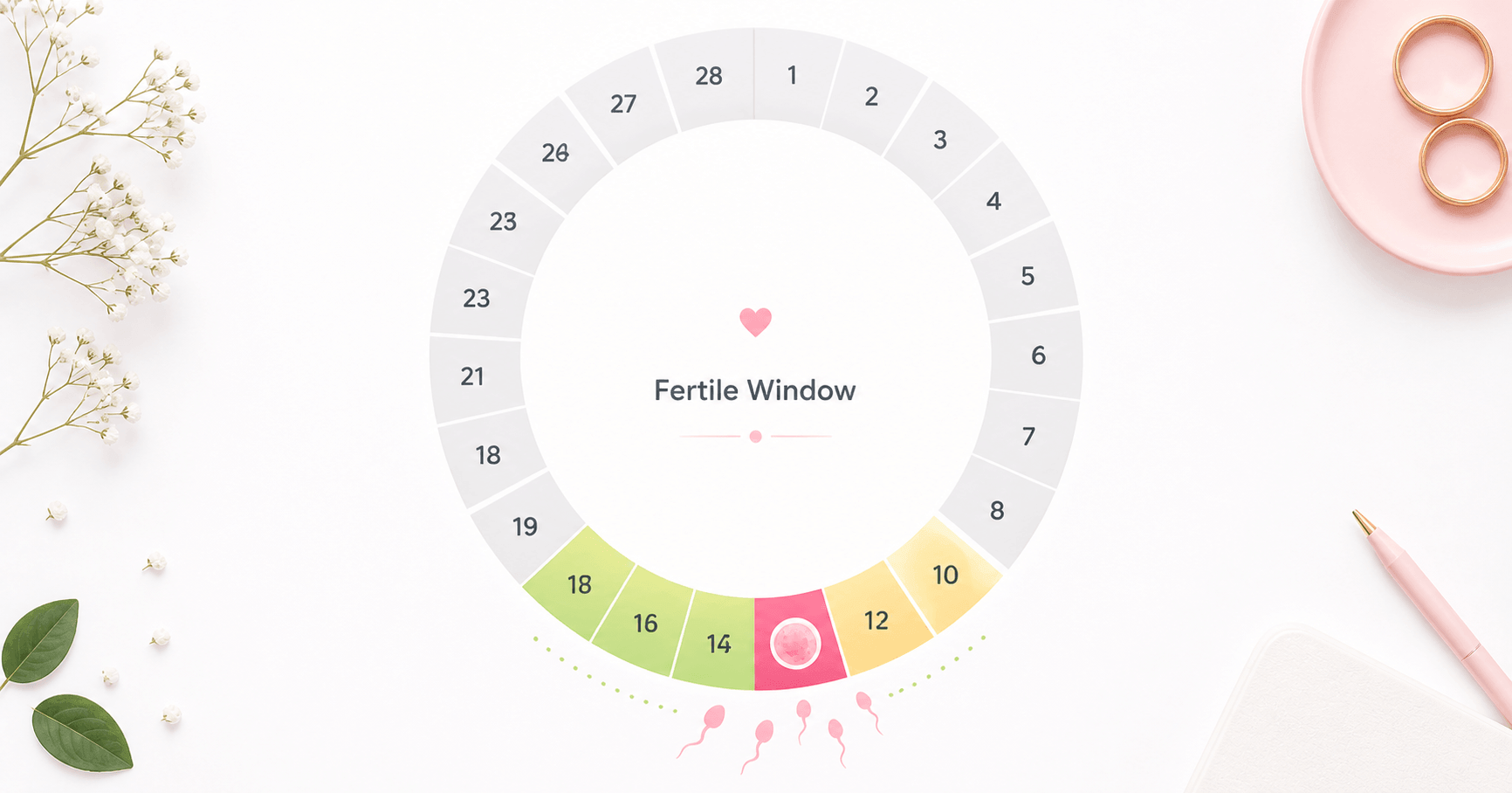
Exactly When in Your Cycle
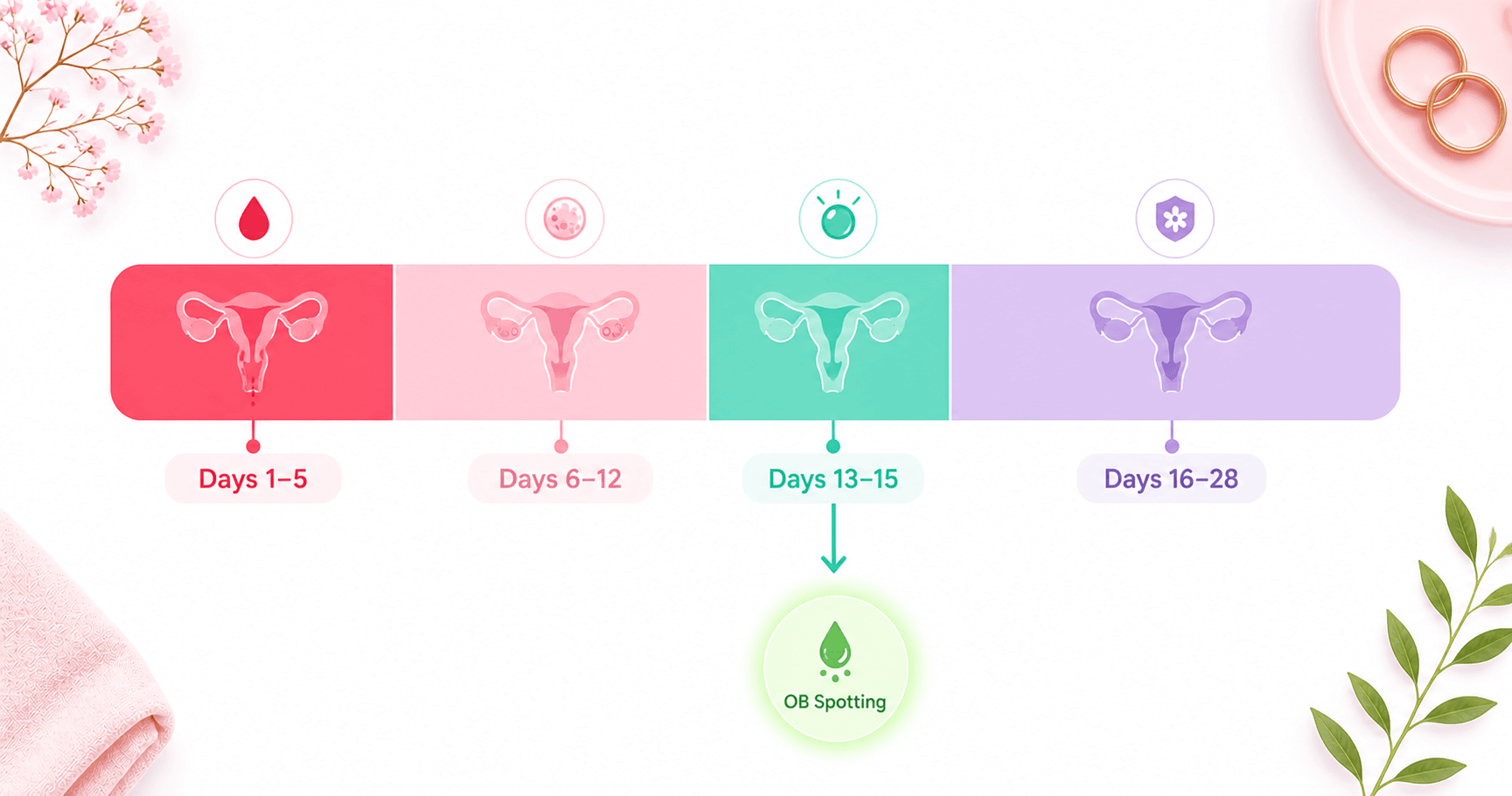
Ovulation bleeding occurs at mid-cycle — specifically when the dominant follicle ruptures. In a textbook 28-day cycle, that is around Day 13–15. But because the luteal phase (from ovulation to the next period) is relatively fixed at 12–14 days, your personal ovulation day scales directly with your cycle length:
← Scroll to see full timeline →
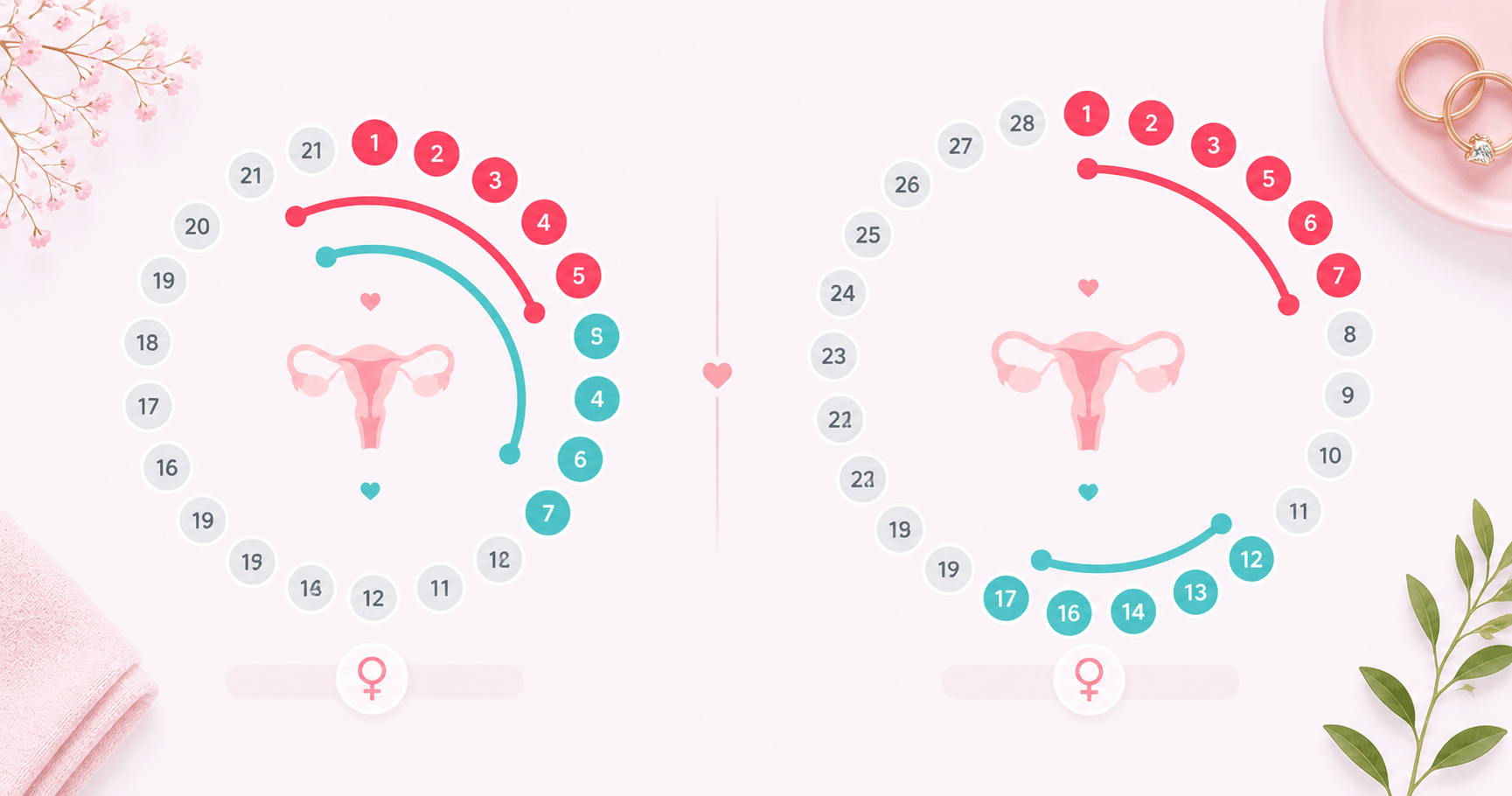
Here is how ovulation spotting timing shifts by cycle length. Shorter cycles mean spotting appears closer to — or even overlapping with — the end of your period:
If your cycle is 21–24 days, ovulation spotting can appear very close to the end of your period — which is one reason short-cycle women often confuse it for spotting at the tail end of their period, or think their period has returned early. For a deep dive on this overlap, see Can You Ovulate During Your Period?
Ovulation Bleeding vs. Implantation Bleeding vs. Period
This is the section most people need. Mid-cycle spotting can look nearly identical to implantation bleeding (early pregnancy) or breakthrough bleeding. The table below breaks down every key difference:
| Feature | Ovulation Spotting | Implantation Bleeding | Period / Breakthrough |
|---|---|---|---|
| Cycle timing | Mid-cycle — Day 13–15 (28-day) | 6–12 days after ovulation — Day 20–26 | Day 1 of new cycle |
| Colour | Pink / pale red / light brown | Light pink or light brown | Bright red → dark red / brown |
| Volume | Trace — barely visible | Trace to very light | Light → heavy flow |
| Duration | Hours to 2 days | 1–3 days | 3–7 days |
| EWCM present? | Yes — often mixed with it | No | No |
| Cramping | Mild (mittelschmerz) or none | None to very mild | Moderate to severe |
| Pregnancy possible? | Not yet — egg just released | Yes — embryo implanting | No |
| Recurrence pattern | Same cycle day every month | Only if pregnant | Every cycle |
The single most useful differentiator: Is the spotting mixed with stretchy, clear egg-white cervical mucus, and does it happen at roughly the same point mid-cycle every month? If yes — ovulation spotting. Implantation bleeding happens later, closer to your expected period date, and does not come with EWCM.
Using Ovulation Bleeding to Confirm Ovulation
Here is the silver lining: consistent ovulation spotting is actually a useful fertility sign. When it appears at the same cycle day each month, it likely indicates your ovaries are releasing an egg reliably — and it can help you time intercourse or verify that ovulation is happening.
Spot + EWCM = Fertile Now
Pink-tinged egg-white mucus is one of the clearest combined signs that you are at or just past peak fertility. This is an excellent time to use an LH strip to confirm the surge.
BBT Rise Confirms It
After ovulation spotting, watch for your basal body temperature to rise by 0.2–0.5°C within 24–48 hours. This temperature shift confirms ovulation occurred and the fertile window has closed.
Log It Every Cycle
Record spotting in your period tracker. After 2–3 cycles you will see whether it consistently appears at your ovulation day — at that point it becomes a reliable personal fertility marker.
Pair with an OPK Strip
Run an LH strip the same day you notice spotting. A positive OPK alongside spotting is very strong confirmation that ovulation is happening right now — perfect timing for trying to conceive.
Track spotting, cervical mucus, LH strip results, and BBT all in one place with Wamiga. The AI learns your personal cycle patterns and identifies your fertile window — including spotting as a fertility signal. Try Wamiga free →
Warning Signs: When Mid-Cycle Spotting Needs Attention
While ovulation bleeding is usually harmless, not all mid-cycle spotting has the same benign cause. See your doctor if you notice any of the following:
Lasts More Than 3 Days
True ovulation spotting resolves within 1–2 days. Mid-cycle spotting lasting 3+ days warrants investigation — cervical polyps, fibroids, or endometriosis can all cause prolonged mid-cycle spotting.
Heavy Mid-Cycle Bleeding
Ovulation spotting is never heavy. If mid-cycle bleeding soaks a pad or liner, that is not ovulation spotting — it requires prompt medical evaluation to rule out structural causes.
Severe Pain Alongside
Mild mittelschmerz (one-sided ovulation cramps) is normal. Intense, doubling-over pain with spotting could indicate an ovarian cyst rupture or, rarely, an ectopic pregnancy — seek urgent care.
Spotting After Sex
Post-coital spotting is not ovulation bleeding. It signals cervical ectropion, polyps, or cervicitis — and in rare cases, early cervical changes. Always report post-sex spotting to your GP.
Also discuss mid-cycle spotting with your doctor if it is a new symptom after previously spotting-free cycles, if it comes with unusual discharge odour, if you are on hormonal contraception (where mid-cycle spotting can signal the need for a dosage review), or if you have been trying to conceive for more than 12 months (6 months if over 35).
For more on the fertile window and what a healthy ovulation timeline looks like, see What Is the Fertile Window? How to Find Yours and What Does Ovulation Discharge Look Like?
Frequently Asked Questions
What does ovulation bleeding look like?
Ovulation bleeding is very light — a pink, pale red, or brownish tinge in your discharge rather than flowing blood. You may notice it on toilet paper or as a faint spot on underwear, and it is often mixed with clear stretchy egg-white cervical mucus. It rarely requires even a thin liner.
How long does ovulation spotting last?
Most ovulation spotting lasts a few hours to 1–2 days. If mid-cycle spotting continues beyond 3 days or becomes heavier than trace amounts, it is not typical ovulation bleeding and should be discussed with your doctor.
Is ovulation bleeding a sign of pregnancy?
No. Ovulation bleeding happens at the moment of ovulation — before any pregnancy is possible. Implantation bleeding, which is an early pregnancy sign, occurs 6–12 days after ovulation (around Days 20–26 in a 28-day cycle) — well after the ovulation window has closed.
Can you confuse ovulation spotting with a period?
Yes, especially on short cycles. If your cycle is 21–24 days, ovulation spotting around Day 7–12 can occur soon after your period ends and feel like it returned early. Tracking your cycle length consistently over several months is the most reliable way to tell them apart.
When should I see a doctor about mid-cycle spotting?
See a doctor if mid-cycle spotting lasts more than 3 days, is heavy enough to require a pad, occurs after sex, comes with significant pain or fever, or is a new symptom after previously regular cycles. These symptoms could point to a polyp, fibroid, cervicitis, or other condition that needs evaluation.